Your Body is
Your Medicine.
Skip the hassle, let us call you!
To learn more about possible treatment options for yourself or family members, schedule an appointment with one of our New Patient Coordinators at a time that works for you!
What Questions Do You Have Today?
I have an injury and I would like to explore options
Take a look at the areas we treat. We have solutions to help with every joint in the body!
I’d like to learn more about a treatment
We are most known for regenerative treatments such as Platelet-rich plasma (PRP) and Stem Cell Therapy. We also perform conventional therapies that are both covered and not covered by your insurance.
I’d like to learn more about our team of providers
Our team of providers are some of the best in the world. They are most known for their ability to diagnose. You should meet them!
I need help accessing the Patient Portal or billing
Or you can call our office at (503) 535-8302

Specialized Treatment Options
In the heart of Lake Oswego, we bring some of the most progressive regenerative medicine options available to you from our world-renowned physicians.

PRP Therapy

Cell Therapy
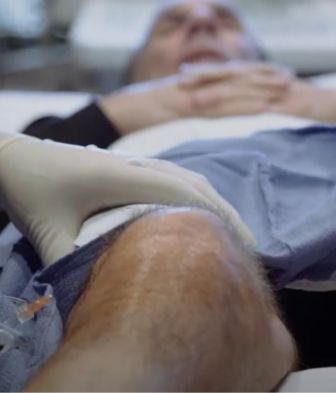
RestoreBLP
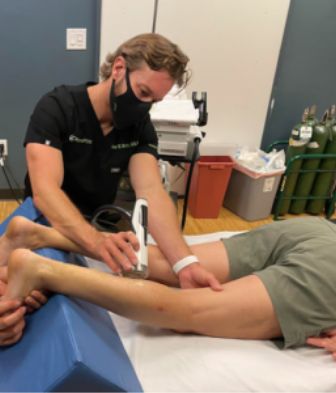
Shockwave Therapy

The TLC Program

For Young Athletes
Our Secret Sauce
Here’s what makes RestorePDX the smarter choice for your health.
Diagnosis
Let’s make sure we know what we’re dealing with, shall we? Our team is all about precision diagnosis as we want to make sure we hit the nail on the head to get you back to your healthy, happy self.
Biologics
We want to make sure that the treatment we give you is the real deal and not just some one-size-fits-all solution. Ask us about some of our innovative biologics such as: RestorePRP, RestoreLipo+PRP, and RestoreBLP.
Delivery
We want to make sure it hits the bullseye every time and delivers the maximum amount of relief. That’s why we use top-of-the-line techniques, like ultrasound and x-ray guidance to make sure we’re injecting the goods exactly where they need to go.
Start Your Journey
Set Up A Consultation
Injuries like joint or tendon pain tell us that your body’s recovery process is stuck. In your consultation, we will get an accurate understanding of what’s happening with your body. We will conduct a thorough physical evaluation and diagnosis, and discuss your health and activity goals.
Receive Your Treatment Plan
We prioritize personalized treatment plans tailored to each individual, offering various options such as conventional pain therapy, shockwave, Cell Therapy, or PRP, to ensure the right treatment for your specific needs.
Schedule Your Treatment
Our care team will assist you in scheduling your treatment, coordinating braces or supplements if necessary, and providing thorough information to ensure optimal outcomes and recovery. All treatments take place in our advanced clinic facility.
Get Answers From an Expert
We actually do things a little differently here at RestorePDX. Rather than waiting on hold for long periods of time or not getting called back at all, have us call you!
We have a new patient coordinator that you can schedule a 10-minute call with.

